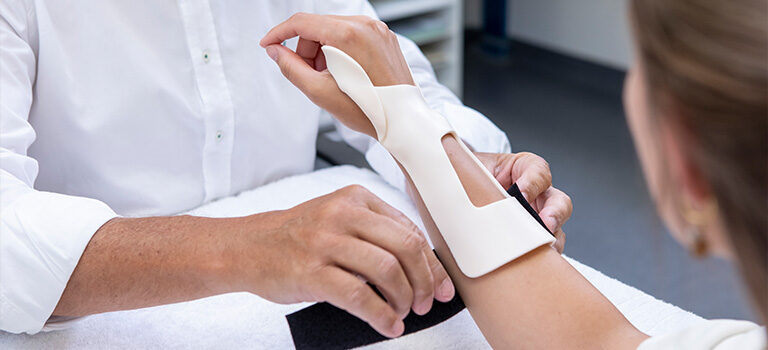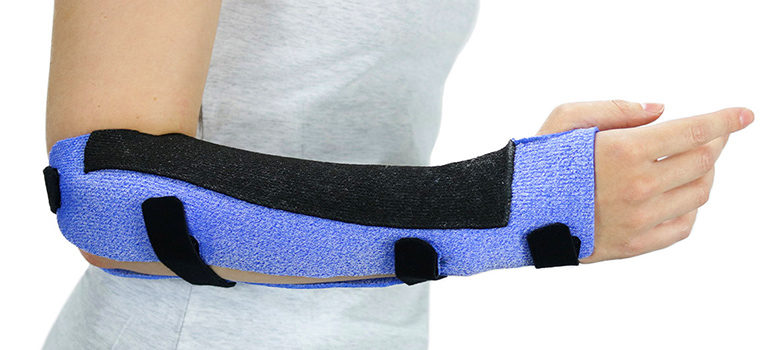
How Effective Are Orthoses for Spasticity?
Orthoses and stretching to reduce post-stroke spasticity
Spasticity is one of the most common motor impairments after a stroke. In general, patients can suffer from joint contractures, muscle shortening, deformities, and pain.
To manage spasticity, therapists routinely use:
- Range of motion (ROM) exercises
- Stretching
- Orthoses
But how effective are these interventions?
A recent systematic review by Kerr et al. (2020), looks to provide guidance. The authors sought and found evidence for the effectiveness of orthoses and stretching to treat post-stroke spasticity.
Orthoses for spasticity: the evidence
The systematic review included 11 studies that had to meet certain inclusion criteria:
- Published between 2004 and 2017 in peer-reviewed journals
- Level I, II, or III studies
- Published in English
All these studies offered evidence for the effectiveness of common splinting interventions for spasticity:
.
Static splinting
The authors found that static splinting can help to reduce spasticity (low strength of evidence), as well as improve hand function and functional task performance (moderate strength of evidence).
Dynamic splinting
The review also indicated that dynamic splinting can increase hand function (moderate strength of evidence).
Stretching devices
Lastly, the authors noted that stretching devices can indeed help at reducing spasticity (strong strength of evidence).
These stretching devices are basically resting hand splints, fitted with adjustable finger components. They are attached to a frame and can hold the stretch for various time increments. However, the long-term effect of these stretching devices is still unknown.
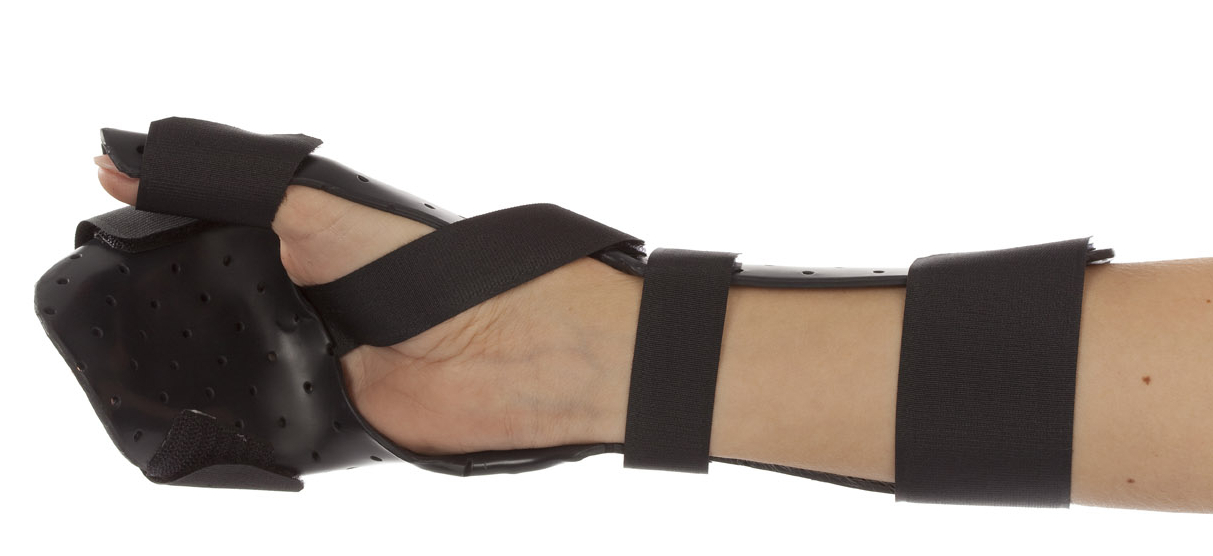
Static orthoses were found to reduce spasticity and improve function.
Implications for treating spasticity
With this review, the authors wanted to provide guidance to therapists on the use of stretching and orthoses. Accordingly, their work came with several implications for the treatment of spasticity:
- Combined interventions: Stretching and splinting should not be used as stand-alone interventions. The evidence indicates that outcomes improve when they are used in combination with additional therapeutic interventions.
- Modifications and adaptations: Stretching and splinting alone may not improve patients’ abilities to perform activities of daily living. Therapists should also consider modifications and adaptations to daily activities to help increase independent functioning.
- Extended period of time: Stretching and splinting need to be ongoing (and may be required for extended periods) for the patient’s maximum benefit.
In summary, there is moderate evidence to support the use of orthoses and stretching to reduce spasticity, increase hand function, and improve functional task performance.
However, the most effective protocol is yet to be determined. More research in this field is therefore required to help clinicians define treatment protocols.
Orthotic fabrication ideas for spasticity
Orthoses for patients with spasticity should be comfortable but also supportive and rigid.
For this reason, Orfit Eco, Orfit Eco Black NS, and Orfibrace are excellent material choices to fabricate orthoses for patients with spasticity. You can use these materials for elbow, resting hand, and wrist orthoses.
And did you know we also offer precuts for resting hand and anti-spasticity orthoses? These precuts can save you both time and effort by eliminating the need for patternmaking.
 |
 |
|
Intrinsic anti-spastic hand orthosis: 35910 / 35911 / 35912 |
Anti-spastic orthosis + thumb piece: 35870 / 35871 / 35872 |
Splinting guides
Many options exist when it comes to splinting for spasticity. Check out the following instruction guides for some suitable designs of static orthoses:
- Tone reducing orthosis for intrinsic muscles or flexor tendons
- Elbow extension orthosis
- Conical resting orthosis
Reference:
![]()

Written by Debby Schwartz, OTD, OTR/L, CHT
Physical Rehabilitation Product and Educational Specialist at Orfit Industries America.
Debby is a certified hand therapist with over 36 years of clinical experience. She completed her Doctorate of Occupational Therapy at Rocky Mountain University of Health Professions in 2010. She has worked at Orfit Industries America as Product and Educational Specialist since 2007.
Debby is also an adjunct professor at the Occupational Therapy Department of Touro University, School of Health Sciences, and at the Occupational Therapy Department at Yeshiva University, Katz School of Science and Health in NYC. She has written many book chapters in the field of hand therapy and multiple articles for hand therapy journals, including the ASHT Times and the Journal of Hand Therapy. She has published a new textbook on orthotic fabrication together with Dr. Katherine Schofield, entitled “Orthotic Design and Fabrication for the Upper Extremity: A Practical Guide”.
![]()
If you’d like to receive the latest product updates and interesting Orfit news, subscribe to our newsletter: